
Polycystic Ovary Syndrome (PCOS) is a multifaceted endocrine disorder affecting millions of women worldwide. Characterized by hormonal imbalances, irregular menstrual cycles, insulin resistance, and metabolic complications, PCOS is more than just a reproductive health issue, it is a chronic condition with long-term health implications. Over the past decade, medical research and pharmaceutical innovation have reshaped the approach to PCOS management, creating a treatment landscape that is dynamic, patient-focused, and rapidly evolving.
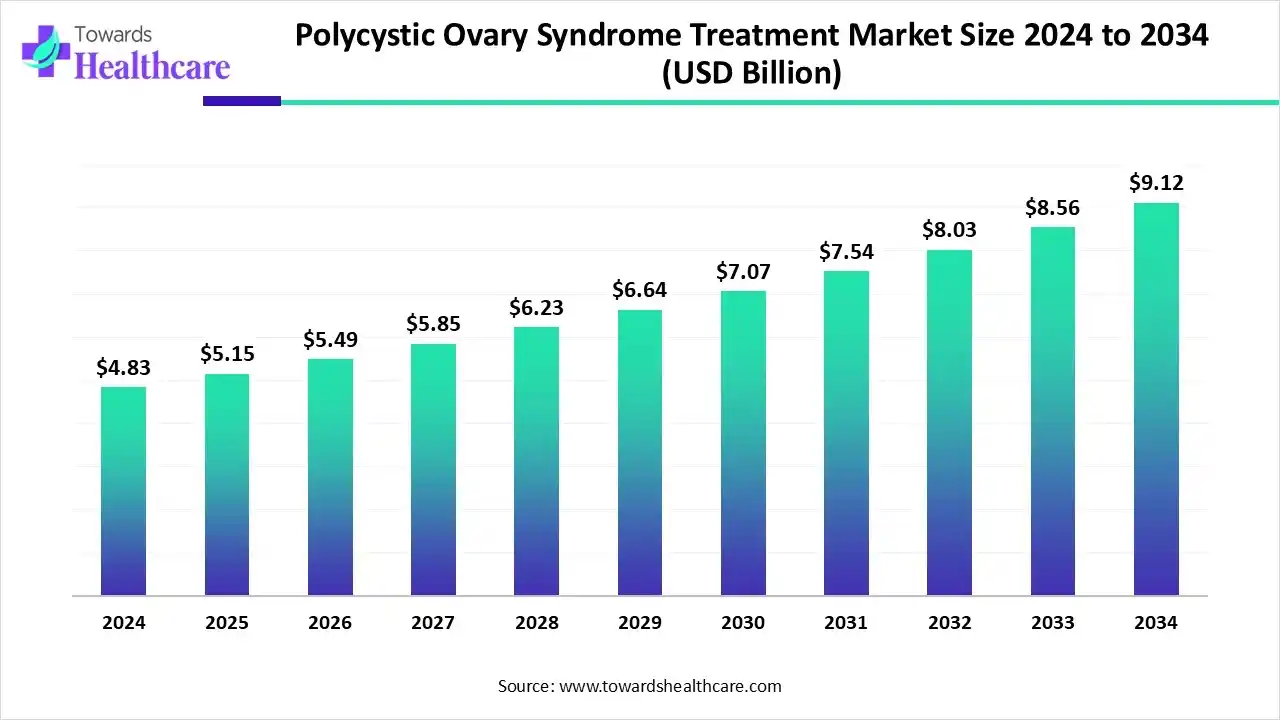
Global Market Dynamics: From $4.83 Billion to $9.12 Billion
In 2024, the global PCOS treatment market was valued at USD 4.83 billion and is projected to reach an impressive USD 9.12 billion by 2034. This represents a steady CAGR of 6.56% between 2025 and 2034, underscoring the market’s strong growth potential. Key drivers include the rising prevalence of PCOS, increasing awareness about women’s health, and the continuous development of innovative therapies. Moreover, government initiatives and global health organizations like the World Health Organization (WHO) are actively promoting research and awareness campaigns, further expanding the market.
Download Sample:
https://www.towardshealthcare.com/download-sample/6252
North America currently leads the global market, benefiting from advanced healthcare infrastructure, early diagnosis, and high patient awareness. Meanwhile, the Asia‑Pacific region is emerging as a hotbed for growth, driven by increasing healthcare access, national health initiatives, and rising public awareness regarding women’s reproductive health. Countries like India and China are witnessing significant investment in research, awareness programs, and digital health interventions to manage PCOS more effectively.
Pharmaceuticals Remain the Backbone of PCOS Management
Among treatment types, pharmaceuticals dominate the market. Hormonal contraceptives, anti-androgens, ovulation induction agents, and insulin-sensitizing drugs like metformin remain frontline interventions. These therapies manage menstrual irregularities, hyperandrogenism, and metabolic complications, improving both fertility and long-term health outcomes. Combination therapy regimens, which integrate multiple pharmacological approaches, are gaining momentum due to their ability to address multiple symptoms simultaneously, including insulin sensitivity, hormonal balance, and weight management.
Oral medications remain the preferred route of administration, largely due to convenience, patient compliance, and the ability to manage multiple symptoms over extended periods. However, injectable fertility agents, such as gonadotropins used in assisted reproductive technologies (ART), are witnessing rapid growth. These treatments cater to women struggling with infertility despite oral therapies, providing advanced solutions through in vitro fertilization (IVF) and intrauterine insemination (IUI).
Adolescents and Young Women Are the Next Growth Drivers
While women of reproductive age continue to constitute the largest patient segment, adolescents and young women are emerging as the fastest-growing demographic. Early diagnosis and intervention are critical to preventing long-term metabolic and reproductive complications. Treatments targeting this group often combine lifestyle interventions with pharmacological therapies to improve insulin sensitivity, reduce androgen levels, and restore regular menstrual cycles.
Lifestyle interventions—including diet modification, exercise, and weight management programs—play a crucial role alongside pharmaceuticals. These approaches are particularly effective in managing metabolic risks and improving overall quality of life. In recent years, personalized care strategies have emphasized integrating lifestyle management with medical treatment, reflecting a holistic approach to PCOS care.
Telemedicine and Digital Health Platforms Transform Care Delivery
The healthcare delivery model is evolving rapidly. Telemedicine and online treatment platforms are projected to grow at the fastest rate within the revenue model segment. These platforms provide remote consultations, treatment monitoring, and behavioral support, improving accessibility and continuity of care for women with PCOS. Digital therapeutics, powered by AI, are enabling personalized care, early diagnosis, and risk assessment, while offering mental and behavioral health support, which is critical given the psychosocial burden of PCOS.
AI algorithms now assist in analyzing hormone profiles, ultrasound images, and genetic markers to predict PCOS risk and tailor treatment plans. Certain startups and digital health firms have raised funding to develop AI-driven platforms empowering women to manage PCOS through digital therapeutics. Similarly, device-based interventions aiming to restore ovulation and improve fertility outcomes reflect a growing emphasis on innovative solutions beyond traditional pharmaceuticals.
The Role of AI in Revolutionizing PCOS Management
Artificial intelligence is playing a transformative role in PCOS diagnosis, treatment, and research. Machine learning models help clinicians identify PCOS earlier and more accurately by analyzing complex datasets, including hormone levels, ultrasound scans, and patient history. AI also assists in risk stratification for related conditions such as diabetes and cardiovascular disease, enabling preventive interventions.
Moreover, AI is accelerating drug discovery and clinical trials by identifying potential therapeutic targets and predicting treatment outcomes. Personalized treatment plans, informed by AI-driven insights, ensure that interventions are tailored to the individual’s hormonal and metabolic profile, enhancing effectiveness and minimizing adverse effects. In the long term, AI has the potential to reshape both patient care and the research landscape for PCOS.
Challenges in PCOS Care and Market Growth
Despite the optimism around growth, several challenges hinder both effective PCOS care and the broader market’s evolution.
1 Diagnostic Inconsistency and Under‑diagnosis
One of the most critical challenges is the lack of uniform diagnostic criteria worldwide. Multiple definitions exist, each with different thresholds for diagnostic markers like hormone levels, menstrual irregularities, and ovarian morphology. This variability leads to inconsistent diagnosis, making it difficult to compare prevalence data across regions or over time. Many women with PCOS remain undiagnosed, and under-diagnosis delays intervention, allowing metabolic and reproductive complications to accumulate over time.
2 High Variability in Prevalence Data
Because of differing diagnostic criteria, ethnic differences, and limited large-scale studies in many regions, prevalence estimates vary widely. Such wide variability complicates public‑health planning, resource allocation, and market forecasting.
3 Limited Awareness and Social Stigma
In many countries, awareness about PCOS remains low. Cultural taboos around menstrual health, body weight, fertility, and hormonal disorders often prevent open discussion. This leads to late diagnosis or misdiagnosis. Moreover, women may attribute symptoms like acne, irregular periods, or weight gain to lifestyle or “bad genes,” delaying medical consultation.
4 Fragmented Care and Inadequate Access
Even where diagnosis occurs, access to comprehensive care — combining lifestyle guidance, hormonal/metabolic therapy, fertility treatment, mental health support — is often limited. Many patients receive only symptomatic treatment without addressing underlying metabolic or psychosocial aspects. In low- and middle-income countries especially, healthcare infrastructure, specialist availability, and affordability pose significant barriers.
5 Adherence & Long-Term Management Issues
PCOS is chronic; it doesn’t “go away.” Managing it often requires long-term commitment to lifestyle changes, regular monitoring of hormones and metabolic markers, possible fertility treatments, and psychological support. Many patients struggle with adherence over time — whether because of lifestyle constraints, financial burden, or lack of support.
6 Research Gaps and Lack of Targeted Therapies
Though research is accelerating, PCOS remains only partially understood. The underlying molecular mechanisms, the interaction between genetics, environment, metabolic health, and lifestyle remain complex. As a result, effective “cures” are lacking; most treatments remain symptomatic or manage complications. Personalized therapies tailored to individual hormonal/metabolic profile are still in early stages.
Potential Solutions & Forward‑Looking Approaches
Overcoming these challenges requires a multipronged strategy — combining improved diagnostics, awareness, research, and holistic care.
1 Standardizing Diagnostic Criteria & Screening Protocols
Global medical bodies should collaborate to harmonize PCOS diagnostic standards. A universally accepted, evidence‑based diagnostic guideline — integrating hormonal evaluation, metabolic assessment, and ovarian imaging — would enable better early detection and consistent data collection. Regular screening programs (especially in adolescents and young women) should be encouraged, so that PCOS can be detected before severe complications arise.
2 Raising Awareness & Reducing Stigma
Public health campaigns must address PCOS like other chronic conditions. Educating women (and men) about PCOS symptoms — irregular periods, acne, weight changes, insulin resistance — and encouraging medical consultation is vital. Schools, colleges, workplaces can play a role by including menstrual and reproductive health education.
3 Promoting Integrated & Holistic Care Models
PCOS management should move beyond isolated drug treatment. Integrated care — including hormonal therapy, metabolic/insulin-sensitivity treatment, nutritional counselling, physical activity guidance, fertility support if needed, and mental health support — should be standard. Telemedicine and digital health platforms can help bridge access gaps, especially in remote areas or regions with limited specialists.
4 Investing in Research & Personalized Medicine
Pharmaceutical and biotech companies, academic institutions, and public health bodies should invest in research exploring molecular mechanisms, genetic predispositions, and individualized treatment approaches. AI and data-driven research offer promise in identifying biomarkers, predicting treatment response, and tailoring therapies.
5 Improving Long-Term Follow-Up & Patient Support
Create support networks — both offline (clinics, support groups) and online (forums, telehealth) — to help patients with adherence, mental health, lifestyle changes, and fertility planning. Regular follow-ups, monitoring metabolic and hormonal markers, and counselling can prevent long-term complications.
Why This Matters: For Patients, Healthcare Systems & the Market
Understanding the scale and complexity of PCOS matters for several reasons:
-
Women’s health as a priority — With an estimated 6–13% of reproductive‑aged women affected globally, PCOS is common. Without proper awareness and treatment, many women risk long-term complications: infertility, metabolic syndrome, diabetes, cardiovascular disease, and mental health issues.
-
Economic and social burden — Chronic management, fertility treatments, and metabolic complications create a long-term healthcare burden. Early diagnosis, prevention strategies, and integrated care can reduce long-term costs.
-
Market opportunity for holistic care and innovation — The growing global burden — coupled with rising awareness — offers opportunities for pharmaceutical, biotech, and digital‑health companies to develop targeted therapies, personalized medicine approaches, AI-driven diagnostics, and telehealth platforms.
-
Need for public health planning and policy interventions — Governments and public health organizations must prioritize PCOS in women’s health policies. Screening programs, awareness campaigns, and funding for research are essential.
-
Empowering patients — Accurate data, standardized care, and integrated support can help individuals make informed decisions about lifestyle, fertility planning, metabolic health, and overall well‑being.
Access our exclusive, data-rich dashboard dedicated to the therapeutic area sector – built specifically for decision-makers, strategists, and industry leaders. The dashboard features comprehensive statistical data, segment-wise market breakdowns, regional performance shares, detailed company profiles, annual updates, and much more. From market sizing to competitive intelligence, this powerful tool is one-stop solution to your gateway.
Access the Dashboard: https://www.towardshealthcare.com/access-dashboard
Checkout Polycystic Ovary Syndrome Treatment Market Report Now at: https://www.towardshealthcare.com/checkout/6252
Become a valued research partner with us – https://www.towardshealthcare.com/schedule-meeting
You can place an order or ask any questions, please feel free to contact us at sales@towardshealthcare.com
Powering Healthcare Leaders with Real-Time Insights: https://www.towardshealthcare.com/healthcare-intelligence-platform
Europe Region – +44 778 256 0738
North America Region – +1 8044 4193 44
APAC Region: +91 9356 9282 04
Visit Our Website: https://www.towardshealthcare.com
Find us on social platforms: LinkedIn | Twitter | Instagram | Medium | Pinterest




