Understanding the Impact of Schizophrenia on Mental Health Disability
Schizophrenia stands as a formidable challenge in the mental health, not only for individuals but also at a population level. Recent research conducted by esteemed professionals sheds light on the profound disability that accompanies this complex disorder. Through meticulous analysis and utilization of extensive medical data, valuable insights have emerged, illuminating the pervasive nature of schizophrenia-related disability.
Unveiling the Findings
Dr. John McGrath, along with a team of experts, delved into the depths of Danish national health registries to unravel the impact of schizophrenia on disability. Their groundbreaking study, published in The Lancet Psychiatry, presents compelling evidence regarding the staggering burden imposed by this condition. By meticulously examining the duration of illness and the degree of disability, researchers revealed that schizophrenia reigns as the most burdensome mental illness, surpassing even alcohol use disorders and anxiety disorders in terms of incapacitation.
Quantifying Disability: Years Lived with Disability (YLD)
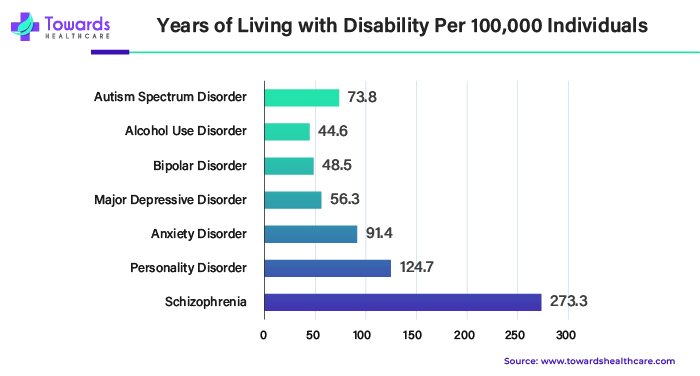
Central to understanding the scope of disability caused by schizophrenia is the concept of Years Lived with Disability (YLD). McGrath and his colleagues leveraged data from the Danish Psychiatric Central Research Register to compute YLD for a spectrum of mental health and substance abuse disorders. This metric, derived by multiplying the duration of illness by a predetermined impairment index, offers a quantitative measure of the disability burden.
Download a short version of this report @ https://www.towardshealthcare.com/personalized-scope/5147
Schizophrenia: A Leading Cause of Impairment
Among the myriad of mental health challenges prevalent in Denmark, schizophrenia emerges as a predominant cause of impairment, transcending gender boundaries. With a profound impact on both men and women, this disorder exacts a significant toll on society, accounting for 273 years of life lost per 100,000 individuals. The sheer magnitude of this statistic underscores the urgent need for comprehensive interventions and support systems to mitigate the consequences of schizophrenia-related disability.
The Complexity of Personality Disorders
In addition to schizophrenia, personality disorders emerge as a significant contributor to disability, standing as the second most incapacitating condition for both sexes. Characterized by enduring patterns of behavior, cognition, and inner experience, personality disorders pose formidable challenges in the realm of mental health. While their impact may vary across individuals, the overarching theme of disability underscores the importance of targeted interventions and holistic treatment approaches.
Addressing the Burden of Anxiety Disorders
Anxiety disorders, prevalent among individuals of all ages and backgrounds, constitute another facet of mental health disability. The intricate interplay between physiological arousal, cognitive distortions, and behavioral responses underscores the complexity of these disorders. As a leading cause of disability, anxiety disorders demand comprehensive strategies encompassing psychotherapy, pharmacotherapy, and lifestyle modifications to alleviate symptoms and enhance overall well-being.
Toward Comprehensive Mental Health Care
The findings underscore the imperative of a multifaceted approach to mental health care, one that transcends traditional boundaries and embraces the complexity of human experience. By integrating insights from research, clinical practice, and lived experiences, stakeholders can collaboratively work towards destigmatizing mental illness and fostering inclusive environments conducive to healing and growth.
The National Institute of Mental Health is actively engaged in conducting various clinical trials aimed at advancing our understanding and treatment of schizophrenia. These trials play a crucial role in driving innovation within the antipsychotic drug industry, establishing the effectiveness of treatments, and shaping clinical practices. Consequently, patients with schizophrenia now have a wider array of treatment options available to them.
Here are some ongoing studies conducted by the National Institute of Mental Health:
- Anti-Inflammatory Challenge in Schizophrenia
- Type of Study: Interventional
- Start Date: March 31, 2024
- Young Adults with Violent Behavior During Early Psychosis
- Type of Study: Interventional
- Start Date: February 29, 2024
- Tau Biomarkers in Late-onset Psychosis
- Type of Study: Observational
- Start Date: February 16, 2024
- Enhanced Coordinated Specialty Care for Early Psychosis
- Type of Study: Interventional
- Start Date: February 1, 2024
- Accelerated Transcranial Magnetic Stimulation for People with Schizophrenia Treated with Clozapine
- Type of Study: Interventional
- Start Date: December 1, 2023
- Auditory Control Enhancement (ACE) in Schizophrenia
- Type of Study: Interventional
- Start Date: September 5, 2023
- Restoring Spindle and Thalamocortical Efficiency in Early-Course Schizophrenia Patients Using Auditory Stimulation
- Type of Study: Interventional
- Start Date: July 20, 2023
- Improving Cognition Through Telehealth Aerobic Exercise and Cognitive Training After a First Schizophrenia Episode
- Type of Study: Interventional
- Start Date: May 23, 2023
- Deep Brain Stimulation in Treatment-Resistant Schizophrenia
- Type of Study: Interventional
- Start Date: March 1, 2023
The Number of Prescribed Antipsychotics has Increased Over the Years
The prescribing of antipsychotic drugs in Ireland saw a notable increase in 2022, as outlined in a research article by MDPI published in January 2024. With Ireland’s population on the rise, reaching 5.15 million by 2022, the number of prescriptions for psycholeptics steadily climbed each year from 2020 onwards. In December 2020, prescriptions peaked at 328,572. By April 2021, at least 31,340 patients were receiving at least one antipsychotic through payment systems. Notably, in 2021, 30.8% of the Irish population was enrolled in the GMS plan, with antipsychotics prescribed to at least 1.9% of the 1.54 million medical card holders. The total ingredient cost of antipsychotics under GMS and DPS programs surpassed USD 26.6 million in 2021.
Subsequent analysis revealed a surge in antipsychotic prescribing within dementia and care home groups, potentially linked to COVID-19 lockdowns and indicative of antipsychotic use in palliative care.
Furthermore, in the United States, the U.S. Department of Health and Human Services noted an increase in the proportion of adults receiving mental health treatment from 2019 to 2021. This rise was particularly notable among adults aged 18-44, where the percentage receiving therapy climbed from 18.5% to 23.2% during the same period. Factors contributing to this increase include heightened awareness of mental health disorders, reduced stigma associated with therapy, improved access facilitated by expanded insurance coverage and teletherapy, and the pandemic’s spotlight on mental health issues.
This upward trend in mental health treatment reflects a positive shift in prioritizing mental well-being, albeit with the acknowledgment of ongoing efforts needed to ensure comprehensive care for all individuals. Additionally, the rise in mental health disorders fuels demand for antipsychotic drugs, necessitating continued research and development to meet the evolving needs of patients and expand treatment options.
The Role of Increase in Product Approvals
In recent years, there has been a notable uptick in research and development, clinical trials, and subsequent approvals of antipsychotic drugs. This trend has notably contributed to the expansion of the antipsychotic drugs market. Scientists are actively engaged in developing innovative therapies aimed at addressing psychotic disorders such as schizophrenia, dementia, bipolar disorders, depression, and other related ailments.
Here are some recent approvals of antipsychotic drugs:
- In January 2024, the FDA greenlit Pimavanserin Capsules (34 mg) and Pimavanserin Tablets (10 mg) for the treatment of hallucinations and delusions associated with Parkinson’s disease psychosis.
- November 2023 saw the FDA accepting Karuna Therapeutics Inc.’s new drug application for KarXT (xanomeline-trospium), intended for treating schizophrenia in adults.
- In May 2023, Otsuka Pharmaceuticals and Lundbeck Inc. secured FDA approval for Rexulti (bexpiprazole) to treat schizophrenia in pediatric patients aged 13-17.
- April 2023 witnessed FDA approval for the extended-release injectable suspension UZEDY (risperidone), developed by MedinCell and Teva Pharmaceuticals, for treating schizophrenia in adults.
- In June 2021, the FDA approved LYBALVI (olanzapine and samidorphan) by Alkermes plc for treating schizophrenia and bipolar disorders.
- December 2021 saw the FDA tentatively approving Zydus Cadila’s Capriprazine for treating schizophrenia and episodes associated with bipolar disorders.
The surge in product approvals is significantly bolstering market growth by introducing advanced and more efficacious drugs for psychosis and its related conditions.
To own our research study instantly, Click here @ https://www.towardshealthcare.com/price/5147
Read More about Antipsychotic Drugs Market:
Unlock Infinite Advantages: Subscribe to Annual Membership
You can place an order or ask any questions, please feel free to contact us at sales@towardshealthcare.com
About Us
Healthcare Web Wire is a premier subsidiary of Towards Healthcare, dedicated to providing comprehensive insights and information related to the healthcare industry. With a commitment to delivering accurate and timely updates, Healthcare Web Wire serves as a vital resource for professionals, enthusiasts, and stakeholders within the healthcare sector. Our platform serves as a central hub for the latest news, trends and developments shaping the healthcare landscape. Join us on Healthcare Web Wire and become part of a vibrant community dedicated to advancing healthcare knowledge and shaping the future of healthcare worldwide.
Explore the comprehensive statistics and insights on healthcare industry data and its associated segmentation: Get a Subscription
For Latest Update Follow Us: https://www.linkedin.com/company/towards-healthcare