Market Momentum: Why AI & ML Dominate
Artificial Intelligence (AI) and Machine Learning (ML) are no longer buzzwords in U.S. healthcare—they are strategic imperatives. The market momentum behind AI is driven by a convergence of economic pressures, regulatory support, technological maturity, and workforce shortages. Let’s break down the driving forces:
Market Growth
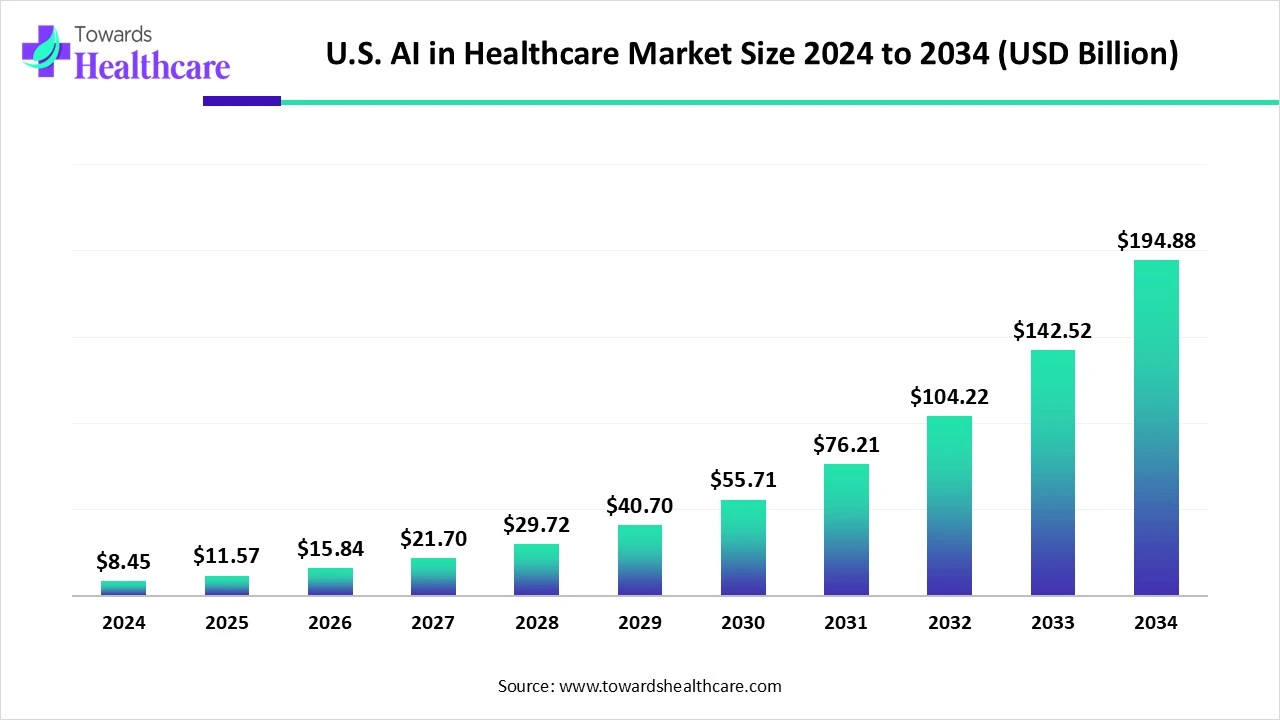
The U.S. AI in healthcare market size stood at US$ 8.45 billion in 2024, grew to US$ 11.57 billion in 2025, and is forecast to reach US$ 194.88 billion by 2034, expanding at a CAGR of 36.97% from 2025 to 2034.
Download the free sample and get the complete insights and forecasts report on this market @ https://www.towardshealthcare.com/download-sample/6024
Key Growth Segments:
➤ Diagnostics: AI is transforming radiology, pathology, dermatology, and ophthalmology by enhancing detection accuracy. For example, AI algorithms can detect breast cancer in mammograms with up to 99% sensitivity, helping to reduce missed cases.
➤Administrative Workflow Automation: AI tools automate scheduling, claims processing, and revenue cycle management. Given that U.S. hospitals spend ~25% of revenue on administrative costs, these solutions directly improve margins.
Why Hospitals are Adopting:
➤The shift to value-based care (VBC) models by payers like CMS (Centers for Medicare & Medicaid Services) has forced providers to deliver better outcomes at lower costs.
➤Hospitals that integrate AI into clinical workflows and operational systems can reduce diagnostic errors, improve staff productivity, and increase revenue capture—all critical to survival in a competitive healthcare environment.
Case Example:
➤Mayo Clinic has piloted AI-driven operational tools that cut ER wait times by 20% and improved imaging turnaround time by 30%. These are not marginal improvements—they are strategic differentiators.
Clinical Integration
➤The conversation has moved from “Will AI be used in hospitals?” to “Where is AI already embedded?”
➤As of 2025, over 40% of U.S. physicians report using AI tools as part of daily workflows.
➤Platforms like OpenEvidence are live in 10,000+ hospitals, proving that AI is no longer limited to research or pilot projects—it is operational.
Key Areas of Integration:
Radiology: AI detects subtle findings in scans (lung nodules, microfractures, hemorrhages) faster than human radiologists.
Oncology: AI assists in tumor classification, genetic testing, and therapy selection.
Cardiology: Algorithms interpret ECGs, echocardiograms, and angiograms with higher sensitivity for early disease detection.
Primary Care: AI triage chatbots guide patients before physician visits, saving time and resources.
Mental Health: AI-based conversational platforms help screen for depression and anxiety, offering support in an understaffed specialty.
Impact on Clinical Workflows:
➤Physicians report time savings of 1–2 hours per day due to AI documentation tools.
➤Hospitals using AI for sepsis prediction models (like those at Johns Hopkins) reduced mortality rates by 18–25%.
Generative AI Surge
➤Generative AI represents the new wave of adoption—and its impact is tangible.
➤By 2025, 85% of U.S. healthcare executives said they were either piloting or scaling generative AI.
Core Applications:
Clinical Documentation
➤Tools like Nuance DAX Copilot generate physician notes automatically during consultations.
➤Early pilots show a 40–60% reduction in time-to-documentation, freeing doctors to focus on patients.
Billing & Coding
➤Generative AI simplifies CPT/ICD code selection and automates insurance claims, reducing errors that cost billions annually.
➤Hospitals using AI billing tools have seen up to 20% improvement in revenue cycle efficiency.
Patient Engagement
➤AI-powered chatbots like Mayo Clinic’s virtual assistant handle routine patient queries, medication reminders, and follow-up care instructions.
➤These reduce call-center volumes by 30–40%, improving patient satisfaction.
Broader Impact:
➤Physician burnout remains a top concern in U.S. healthcare, with over 50% of clinicians reporting high levels of stress. Generative AI, by eliminating repetitive tasks, is directly tied to workforce well-being.
Regulatory Greenlight
➤Historically, regulatory uncertainty slowed AI adoption in healthcare. That barrier has largely eroded.
➤The FDA has approved more than 500 AI/ML-enabled medical devices by 2025.
These approvals span:
Diagnostic Imaging: MRI, CT, mammography AI tools.
Digital Pathology: Whole-slide imaging AI systems.
Cardiology: AI-assisted ECG interpretation devices.
Neurology: Stroke triage algorithms.
Remote Monitoring: Wearable-based cardiac arrhythmia detection.
Why This Matters:
➤FDA approval provides validation of safety and efficacy, lowering adoption risk for providers.
➤Investors gain confidence, accelerating funding into AI startups. In 2025 alone, healthcare AI startups raised over USD 7 billion in venture capital.
Forward-Looking Regulatory Trends:
➤The FDA has proposed frameworks for continuous learning systems, where AI models can update after deployment under “pre-certified” pathways. This will allow faster innovation cycles without re-approval delays.
Workforce Need
➤The U.S. healthcare workforce is facing an existential challenge.
➤The Association of American Medical Colleges (AAMC) projects a shortage of 86,000 physicians by 2036, alongside nursing and allied health gaps.
How AI Bridges the Gap:
Automating Triage: AI chatbots and virtual nurses handle pre-visit questions and direct patients to appropriate care settings.
Decision Support: AI helps physicians interpret complex test results quickly, reducing diagnostic delays.
Force Multiplier for Nurses: AI-enabled monitoring systems alert staff to patient deterioration, allowing fewer nurses to safely oversee more patients.
Implications for Hospitals:
➤Facilities that integrate AI will attract talent by reducing burnout and workload.
➤Those that resist adoption may face staff attrition, worsening shortages, and ultimately a competitive disadvantage.
Case Example:
Mount Sinai Health System has deployed AI-driven clinical decision support that reduces unnecessary testing by 15%, allowing physicians to see more patients without compromising care quality.
Machine Learning: The Backbone of AI in Healthcare
Real-World Deployments of ML in U.S. Healthcare
AI and ML are no longer theoretical—they are actively transforming care delivery in major health systems and networks across the U.S. Hospitals and healthcare providers are leveraging AI to improve diagnostic accuracy, streamline operations, and enhance patient engagement.
Cleveland Clinic (2025) – AI-Powered EEG Monitoring
Deployment: Cleveland Clinic implemented AI algorithms in ICU EEG monitoring systems to detect seizures in real time.
Impact:
➤AI identifies seizure activity within seconds, compared to manual detection which may take minutes or longer.
➤Enables ICU staff to respond faster to life-threatening neurological events, improving patient survival and reducing complications.
Broader Implication: This deployment demonstrates how AI augments critical care, reducing human error and workload, while providing actionable insights in high-stakes environments.
RadNet DeepHealth (2025) – Population-Scale AI Screening
Deployment: RadNet launched next-generation AI screening tools for radiology, enabling automated analysis of mammograms, CT scans, and X-rays across thousands of patients.
Impact:
➤Reduces missed diagnoses by flagging subtle anomalies that human radiologists may overlook.
➤Accelerates workflow efficiency by prioritizing urgent cases.
Broader Implication: Demonstrates the potential for population health management, enabling hospitals and payers to identify at-risk patients proactively, and paving the way for predictive care models.
PracticeSuite (2025) – AI-Driven Administrative Automation
Deployment: PracticeSuite rolled out cloud-based AI systems for automating clinical documentation, claims processing, and billing workflows.
Impact:
➤Reduced administrative time by up to 30–40%, allowing staff to focus on patient-facing tasks.
➤Improved billing accuracy, reducing denied claims and lost revenue.
Broader Implication: Highlights how AI is not limited to clinical care—administrative AI directly improves operational efficiency and financial performance.
Hippocratic AI & Universal Health Services (2025) – AI Agents for Patient Outreach
Deployment: Generative AI agents were deployed to handle post-discharge patient follow-up, medication reminders, and symptom monitoring.
Impact:
➤Increased patient engagement and adherence to care plans.
➤Reduced 30-day readmission rates, a key metric for value-based care reimbursements.
Broader Implication: Demonstrates how AI can extend care beyond hospital walls, improving long-term outcomes and patient satisfaction.
Challenges Ahead
Despite promising deployments, AI adoption in U.S. healthcare is not without hurdles. Successful scaling requires addressing technological, regulatory, and human factors.
Data Privacy
HIPAA Compliance: Strict federal regulations govern patient data storage, sharing, and usage. AI systems, particularly cloud-based solutions, must ensure end-to-end encryption, secure access controls, and audit trails.
Emerging State Laws: States such as California and New York are drafting AI-specific healthcare data regulations, increasing the complexity of compliance.
Implication: Failure to comply risks financial penalties, reputational damage, and legal exposure. AI vendors and health systems must prioritize privacy-by-design architectures.
Clinician Skepticism
Accuracy Concerns: Clinicians worry AI may misdiagnose rare or complex conditions, especially where historical training data is limited.
Liability Risks: Questions remain over who is legally responsible if AI provides incorrect recommendations leading to adverse outcomes.
Workflow Disruption: Integrating AI tools into existing EHRs and clinical routines can cause friction if interfaces are not intuitive or interoperable.
Impact: Adoption may be slowed without robust clinical validation studies, clear liability frameworks, and user-friendly integration.
Ethical Oversight
AI-Only Therapy Bans: In 2025, Illinois enacted legislation prohibiting AI-only treatment without human supervision, reflecting concerns over safety, accountability, and clinical judgment.
Bias and Equity: AI models trained on unrepresentative datasets may produce disparate outcomes for minority populations, exacerbating healthcare inequities.
Implication: Ethical governance frameworks, algorithmic audits, and human-in-the-loop oversight are essential to safe deployment.
ROI Pressure
Financial Justification: Hospitals are cautious, demanding tangible cost savings and operational improvements before committing to AI solutions.
Performance Metrics: AI vendors must demonstrate measurable impact—reduced errors, faster documentation, improved patient outcomes, or revenue enhancement.
Strategic Implication: Without clear ROI, adoption may remain fragmented, limited to academic hospitals or large integrated delivery networks.
Additional Challenges
Interoperability: AI tools must integrate seamlessly with multiple EHRs, lab systems, and imaging platforms.
Training and Adoption: Clinicians require ongoing training and support to trust and effectively use AI systems.
Cybersecurity Risks: As AI increasingly relies on cloud infrastructure, the threat of data breaches and ransomware attacks grows.
Opportunities for Growth
The next wave of AI adoption in U.S. healthcare will be driven by scaling, personalization, and deeper integration into clinical and operational workflows. Hospitals, payers, and tech providers are increasingly looking for solutions that deliver measurable value, enhance efficiency, and improve patient outcomes.
Generative AI Scaling
Generative AI represents a transformative opportunity across clinical, administrative, and patient-facing functions.
Applications and Impact:
Clinical Documentation: AI scribes (like Nuance DAX Copilot) generate SOAP notes, procedure summaries, and discharge instructions automatically during physician-patient interactions. Early studies show:
Time savings: Physicians can save 1–2 hours per day, reducing burnout.
Improved accuracy: Standardized notes reduce transcription errors and inconsistencies.
Billing and Coding: Automated assignment of CPT/ICD codes reduces denials and improves revenue cycle efficiency. Hospitals report 10–20% faster claim processing after AI integration.
Patient Engagement: AI-driven chatbots handle appointment scheduling, symptom triage, medication reminders, and follow-ups, reducing the need for manual call-center intervention.
Economic Potential:
➤U.S. hospitals spend billions annually on administrative tasks (~25–30% of revenue). Generative AI could save several billion dollars annually by streamlining documentation and operational workflows.
➤By reducing repetitive tasks, AI also enhances clinician satisfaction, which is critical given the ongoing workforce shortage.
Strategic Implications:
➤Organizations that scale generative AI effectively can integrate it across specialties, improving efficiency across the entire care continuum.
➤Continuous learning capabilities allow AI to adapt to specialty-specific language and workflows, further enhancing accuracy and adoption.
Drug Discovery Acceleration
➤AI is revolutionizing the pharmaceutical and biotech sector, accelerating drug discovery and development.
Key Transformations:
➤Candidate Identification: ML algorithms analyze molecular structures, biological pathways, and prior research to identify promising drug candidates faster than traditional methods.
➤Trial Optimization: Predictive analytics improves patient selection, protocol design, and adherence monitoring, reducing recruitment timelines by up to 40%.
➤Biomarker Discovery: AI detects novel biomarkers for targeted therapies, enabling precision medicine approaches.
Partnerships Driving Innovation:
➤Collaborations like NVIDIA–Medtronic and Microsoft–Novartis are leveraging AI to enhance R&D pipelines, from preclinical research to clinical trial execution.
➤Startups are also integrating with pharma for AI-driven drug repurposing, reducing development costs and time-to-market.
Economic and Clinical Implications:
➤Faster, data-driven drug discovery reduces development costs by hundreds of millions per drug.
➤Patients gain earlier access to innovative therapies, improving survival rates and quality of life.
Ambient Clinical Support
➤Ambient AI refers to voice-enabled, context-aware assistants embedded in clinical workflows.
Applications and Impact:
➤AI assistants listen during consultations, automatically documenting notes, coding procedures, and generating clinical summaries.
➤Physicians regain up to 2 hours per day previously spent on documentation.
➤Reduces errors from manual transcription, ensuring accurate patient records.
Examples:
➤Nuance DAX Copilot and similar platforms are now integrated into Epic and Cerner EHRs, providing real-time, specialty-specific documentation.
➤Some hospitals report 20–30% reduction in charting time, freeing clinicians for direct patient care.
Strategic Advantage:
➤Ambient AI supports hospitals in addressing physician burnout, a major factor in workforce attrition.
➤When scaled across departments, it enables uniform documentation standards, facilitating regulatory compliance and research data quality.
Value-Based Care Alignment
➤AI and ML are essential enablers for value-based care (VBC) models, which focus on outcomes per dollar spent.
Applications:
➤Predictive Analytics: Identifies patients at risk for hospitalization, complications, or chronic disease progression, allowing for preventive interventions.
➤Operational Optimization: AI forecasts resource utilization, reducing unnecessary tests, bed occupancy, and staffing inefficiencies.
➤Payment Modeling: ML predicts reimbursement eligibility and optimizes claims processing, aligning financial incentives with patient outcomes.
Impact:
Hospitals adopting AI for VBC report 15–25% improvements in patient outcomes metrics and measurable cost reductions.
AI facilitates personalized care pathways, ensuring interventions are effective and efficient, directly supporting payer goals.
Future Outlook: AI-First Healthcare by 2034
By 2034, the U.S. healthcare system is expected to transition into an AI-first model, where AI and ML are integral to every aspect of care delivery, operations, and payment models.
Hospitals
➤AI-driven triage systems will analyze patient symptoms, history, and vitals to prioritize care efficiently.
➤Near-zero diagnostic error rates will become the standard in radiology, pathology, and cardiology, supported by continuous learning algorithms.
➤Clinical decision support will become real-time, predictive, and prescriptive, guiding clinicians toward optimal interventions.
Labs and Diagnostics
➤Fully automated imaging and pathology workflows will dominate, with AI pre-interpreting scans and slides for human review.
➤ML will continuously update protocols based on new evidence, creating self-improving laboratory operations.
➤Turnaround times for diagnostics will be reduced dramatically, supporting faster treatment decisions.
Payers
➤Machine learning will guide real-time reimbursement decisions, adjusting payments based on predicted patient outcomes and resource utilization.
➤Payers will leverage predictive models to incentivize preventive care and reduce avoidable hospitalizations.
➤Value-based contracts will increasingly rely on AI-generated evidence to measure outcomes and optimize costs.
Tech–Provider Partnerships
➤Collaborations such as Microsoft–Epic and NVIDIA–Medtronic will define industry standards, integrating AI deeply into EHRs, imaging platforms, and surgical robotics.
➤AI infrastructure will become modular and interoperable, allowing hospitals of all sizes to access high-performance AI tools.
➤Startups and established tech firms will jointly develop next-gen clinical AI, accelerating innovation cycles.
Patient Experience
➤Personalized AI-driven care navigation will guide patients through appointments, treatments, and follow-ups.
➤AI will continuously analyze patient data to recommend lifestyle interventions, preventive care, and early treatments.
➤Patients will experience higher satisfaction, better outcomes, and lower costs, as care becomes more predictive, personalized, and precise.
Strategic Implications
➤By 2034, AI and ML will shift from supporting roles to core infrastructure in U.S. healthcare.
➤Hospitals that adopt AI early will gain operational efficiency, improved patient outcomes, and competitive advantage.
➤Tech–provider partnerships and ethical deployment frameworks will shape the standard of care, ensuring AI benefits are equitably distributed.
Top 5 Most Searched Queries
1. What is driving the rapid growth of AI and ML in U.S. healthcare?
Answer:
AI and ML are growing rapidly due to a combination of factors:
The U.S. AI healthcare market is projected to grow from USD 11.57 billion in 2025 to over USD 194 billion by 2034.
High-impact areas like diagnostics and administrative workflow automation are improving accuracy and efficiency.
Physician shortages, regulatory approvals (500+ FDA-cleared devices by 2025), and the shift to value-based care are driving adoption.
2. How is machine learning used in clinical practice?
Answer:
Machine learning powers data-driven precision and continuous improvement across healthcare:
Diagnostics: Early detection of cancers, cardiovascular disease, and neurological conditions.
Population Health: Risk stratification to guide preventive interventions.
Genomics and Clinical Trials: Accelerates variant interpretation and patient recruitment.
Continuous Learning: ML models improve accuracy over time as they process new data.
3. Which companies are leading AI & ML adoption in U.S. healthcare?
Answer:
The leading players include:
IBM Watson Health: Oncology and imaging decision support.
Google Health (DeepMind): AI in imaging and predictive care integration.
Microsoft Healthcare: Generative AI for documentation, Epic EHR integration.
AWS Healthcare: Data lake solutions for predictive analytics.
NVIDIA, Tempus Labs, PathAI: AI for imaging, genomics, and pathology.
These companies provide platforms, cloud infrastructure, and AI tools that hospitals, labs, and pharma are using to scale AI-driven solutions.
4. What are the main challenges limiting AI adoption in healthcare?
Answer:
Key barriers include:
Data Privacy: HIPAA compliance and emerging state AI data laws.
Clinician Skepticism: Concerns about accuracy, liability, and workflow disruption.
Ethical Oversight: Bias in AI models and bans on AI-only therapy (e.g., Illinois 2025).
ROI Pressure: Hospitals demand measurable improvements in cost, efficiency, and patient outcomes.
5. What does the future of AI in U.S. healthcare look like by 2034?
Answer:
By 2034, AI and ML will be central to healthcare delivery:
Hospitals: AI-driven triage, near-zero diagnostic errors.
Labs: Fully automated imaging and pathology workflows.
Payers: ML-guided real-time reimbursement and preventive care.
Patient Experience: Personalized, AI-powered care navigation.
Tech–Provider Partnerships: Collaborations like Microsoft–Epic and NVIDIA–Medtronic will define interoperability and innovation standards.
Access our exclusive, data-rich dashboard dedicated to the healthcare market – built specifically for decision-makers, strategists, and industry leaders. The dashboard features comprehensive statistical data, segment-wise market breakdowns, regional performance shares, detailed company profiles, annual updates, and much more. From market sizing to competitive intelligence, this powerful tool is one-stop solution to your gateway.
Access the Dashboard: https://www.towardshealthcare.com/access-dashboard
Immediate Delivery Available | Buy This Premium Research @ https://www.towardshealthcare.com/price/6024
Become a valued research partner with us – https://www.towardshealthcare.com/schedule-meeting
You can place an order or ask any questions, please feel free to contact us at sales@towardshealthcare.com
Powering Healthcare Leaders with Real-Time Insights: https://www.towardshealthcare.com/healthcare-intelligence-platform
Europe Region – +44 778 256 0738
North America Region – +1 8044 4193 44
APAC Region: +91 9356 9282 04
Web: https://www.towardshealthcare.com
Find us on social platforms: LinkedIn | Twitter | Instagram | Medium | Pinterest